A 32 year old software professional was suffering with severe low back pain and radiating pain in both the legs. He was unable to stand straight and could not walk more than a few metres due to the pain.
His MRI revealed a large disc prolapse at L3-L4 level causing significant nerve root compression causing his symptoms and there was a significant risk of further worsening, affecting the nerve function causing paralysis in lower limbs as well as his bladder and bowel control. It was clear that he needed a surgery to release the compression on the nerves
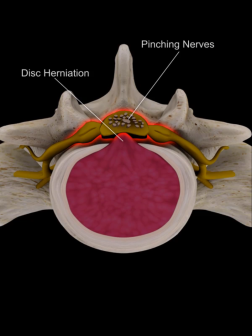
But he was pronounced to be a high risk candidate for anaesthesia due to his morbid obesity and impaired lung function. It meant that he had a high risk of needing ventilatory support if he was put under general anaesthesia as his morbid obesity might hamper his recovery while reversing the anaesthesia.
An Endoscopic disc surgery under local anaesthesia through a transforaminal approach was considered the most suitable option for him as it avoids the need for general anaesthesia. Although a transforaminal endoscopic disc surgery is a routinely done procedure, morbid obesity in this particular patient presented certain unique challenges.
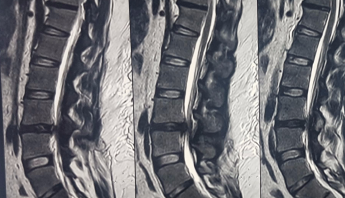
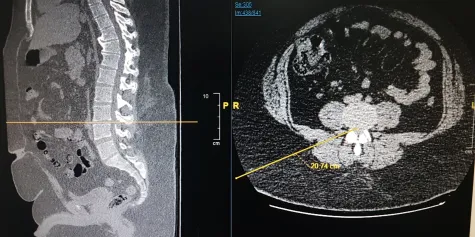
Despite the above mentioned challenges, the procedure was successfully carried out as the patient could tolerate the prone position long enough to complete the surgery. The length of the scope was just enough to reach the targetarea and there was enough visualisation of the spine with the image intensifier. The patient was awake throughout the procedure and was comfortable and communicating with the surgeon during the entire duration of the surgical procedure.
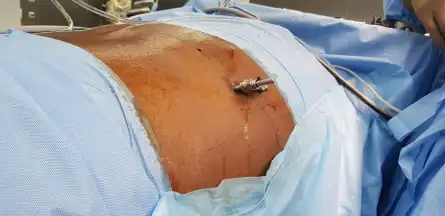
The patient had immediate pain relief and was able to walk without the leg pain and with straight posture within a few hours after the procedure. He was discharged from the hospital the next day. He recovered rapidly and was back to work within four weeks.
This case beautifully emphasises the advantages of an endoscopic disc surgery in terms of avoiding general anaesthesia and attaining the desired results safely while enabling a fast recovery and return to work in patients at high risk of complications with conventional open disc surgery.
If you liked the article, please share it and subscribe to my future articles on spine problems. Thank you.!

With years of experience in spine surgery, Dr Phani Kiran S, Senior Consultant Spine Surgeon will assess you and suggest the treatment option that is right for you.
We at Medspine clinics, understand the importance of educating all our patients about the spinal problems and the most effective ways to take care of their spine.
The Ortho Clinic: Monday, Wednesday, Friday, Saturday.
Ojas Health: Tuesday, Thursday
© Copyright 2024 MedSpine. All Rights Reserved. Build with 🤍 by Digital GYB
WhatsApp us